Hello turdburgler and All, I have bradycardia (slow heart rate) and also now have a pacemaker to provide a ‘floor’ for my heart rate so it will not beat too slowly.
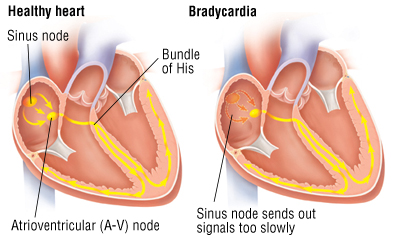
The pacemaker function is transparent to me (I am not aware of it at all) and my heart rate goes up normally during exercise and returns to normal as before ….. but the pacemaker prevents my heart from going too slowly when resting or sleeping.
Could it be that some young highly trained individuals have heart rates that are pumping ‘too’ slowly when sleeping or resting? https://www.ncbi.nlm.nih.gov/...articles/PMC4024745/ Excerpts:
After lifelong physical endurance training, veteran endurance athletes have a higher incidence of sinus node disease and artificial pacemaker implantation than normal individuals
5,
6,
7, and it is likely that this is a consequence of the marked remodelling of the sinus node shown here.
It may also help explain syncope [fainting] in the young athlete
46. Other rhythm disturbances beset the athlete (for example, atrial fibrillation, heart block
47,
48, bundle branch block
48,
49 and
even sudden cardiac death50,
51) and it is likely that they are a consequence of an analogous remodelling of other parts of the heart: the atrial muscle, atrioventricular node, Purkinje fibres and ventricles (perhaps in combination with a
pre-existing heart condition in the case of sudden cardiac death). [added or emphasis]
Exercise is undoubtedly beneficial for the cardiovascular system, but at the same time intense endurance training can have harmful effects, and our findings highlight the fundamental changes taking place.
https://www.ncbi.nlm.nih.gov/...articles/PMC4405729/ It is well known that athletes have a low resting heart rate (bradycardia). The bradycardia can be moderate to severe: reports of heart rates of 40–60 beats min−1 in athletes are common (Boyett
et al.
2013), and Jensen-Urstad
et al. (
1997) reported heart rates of <30 beats min−1 in elite athletes at night. Consistent with this, S. Sharma has studied 142 elite cyclists and rowers and observed heart rates over the range 30–70 beats min−1; the distribution of heart rates in the athletes (and for comparison in a normal population) is shown in Fig.
Fig.1.1.
The resting heart rate is easy to measure and it is clear that athletes use the resting heart rate as a measure of fitness and speak of it in terms of pride and bravado. This is despite evidence that veteran athletes are more likely to need an electronic heart pacemaker fitted in later life (Baldesberger et al. 2008). [emphasis added]
The bradycardia is widely believed to be the result of high vagal tone; this is a natural assumption because high vagal tone will reduce the heart rate. However, despite this widespread belief, efferent vagal nerve activity to the heart's pacemaker (the sinus node) has never been recorded. It is not obvious how it could be measured, because the vagus nerve carries afferent as well as efferent nerve fibres. Because of this, the scientific community uses what is assumed to be a surrogate of vagal nerve activity to the sinus node, heart rate variability.
Heart rate variability is a beat-to-beat variability in the heart rate and is assumed to be the result of stochastic fluctuations in autonomic nerve activity to the sinus node and changes in heart rate variability are assumed to represent changes in this. PubMed lists more than 17,000 publications concerned with heart rate variability.
Heart rate variability is higher in athletes (Aubert
et al.
2003) and this is taken as evidence of high vagal tone in athletes, and this is then assumed to be responsible for the bradycardia. However, a causative link between autonomic nerve activity and heart rate variability has never been demonstrated (for reasons discussed above). Furthermore, we have recently analysed the biophysics underlying heart rate variability and we have shown that, regardless of whatever is responsible for heart rate variability, heart rate variability is a steep exponential function of heart rate (heart rate variability increases with a decrease in heart rate) and the majority of reported changes in heart rate variability can be explained by the concurrent change in heart rate (Monfredi
et al.
2014).
https://www.ncbi.nlm.nih.gov/pubmed/23657540 https://www.ncbi.nlm.nih.gov/pubmed/24886917 https://www.ncbi.nlm.nih.gov/pubmed/18512181 https://www.ncbi.nlm.nih.gov/pubmed/14992127
Cheers, Neal
+1 mph Faster

