Toby wrote:
Mark Lemmon wrote:
Definitely concerning for this 58 year old too. I think the growing trend of time trial starts might help reduce the number of issues with competitors who go way too hard at the start of the swim. RDs should also promote swim warm ups at their events and ensure that participants always have a place to warm up in the water within 15 minutes of their starting time.
Heh, concerning for me too, at 56 years old, and with a very significant cardiac history in my family...although that isn't why I went into cardiology.
I think it's a very good longitudinal study. Hopefully will continue to shine the light on the fact that CAD is still number one in terms of risk of dying, after the age of 35 years (male or female). I also think the press has sensationalized it a bit, as often happens. Awareness is good. Scaring people away from engaging in activities that keep them fit is bad, IMO.
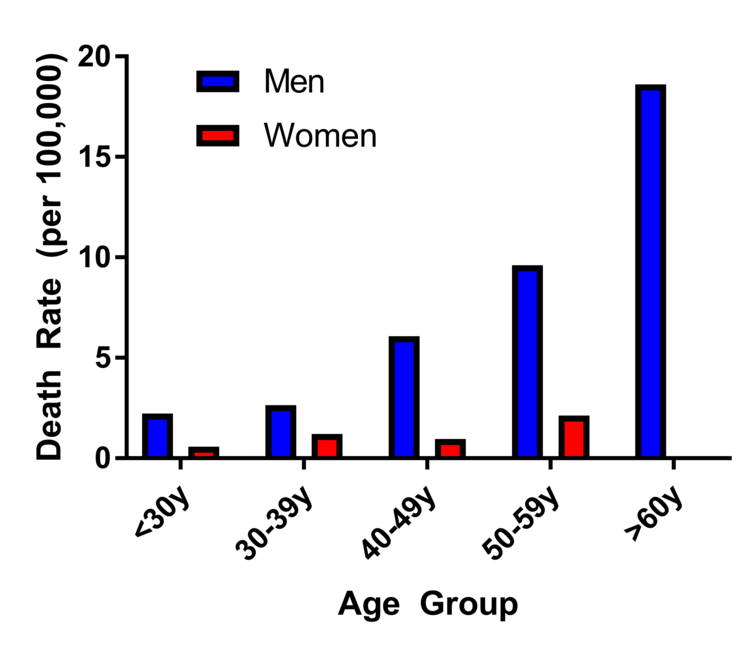
https://www.cdc.gov/...ets/fs_men_heart.htm Looking at the CDC data from a few years ago, rates are ~500/100,000 people. That is just a tad bit higher than 14/~100,000 participants in a USAT triathlon race. The quoted SCD rate was 1.2/100,000 which is in line with previously documented SCD rates in marathon runners. And risk always goes up with age so 60 yo males will certainly have more risk than 40 yo males.
What is bothersome to me is that it is entirely possible that a considerable number of relatively 'new to the sport' people may be in this group of SCD (sudden cardiac death). How to find and screen them...how to reassure the rest...how to make sure RD's are maximally aware to have everything in place to give a potential victim at their race the best chance of survival...It is notable that SCD appears to be significantly higher in triathlon than in marathon running.
What we don't know is what these people actually had for risk profiles for CAD and if they had symptoms of concern. What was their cholesterol numbers? Did they even see their PCP and tell them they were training for an upcoming triathlon. Should we be screening people a bit more aggressively for heart disease? That is a good question. You have to understand though, that activity is indirectly proportional to your risk of heart disease and an event. The more active you are, the less likely you will have clinically significant heart disease and die from it.
From 'Up to date'.
COMPETITIVE ATHLETES
Incidence of sudden death — It is widely acknowledged that SCD is the leading medical cause of death in athletes, although its exact incidence remains unclear. Data are imprecise since most are derived from retrospective analyses, and incidence varies depending upon the intensity of exercise, the athletic population considered, and the time period of observation (figure 1) [4-8]. Use of media reports or catastrophic insurance claims as the primary method for case identification underestimates the risk of SCD in athletes. The best available evidence, together with a close examination of reporting methods for case identification and population definitions, suggests that the incidence of SCD in athletes is higher than initial estimates. An overall incidence of 1:50,000 per year in young athletes is a reasonable estimate based on existing information from retrospective cohort studies and prospective observational and cross-sectional studies. Male athletes are consistently found to be at greater risk, and there appears to be a disproportionately higher risk among male African-American athletes.
The magnitude of the problem and the challenges inherent in screening are illustrated in reports of arrhythmic events associated with major endurance sporting events [6,9].
For practical purposes, we consider here the largest study examining prevalence of SCD in 215,413 marathon runners participating in a Marine Corps, or a civilian marathon over a 19-year period [6]. The following findings were noted:
●SCD occurred in four individuals during or immediately following the marathon, an incidence of approximately 1 in 50,000. This is substantially lower than the annual risk of premature death in the general population.
●None of the four subjects had prior cardiac symptoms.
●Two of the four had completed several previous marathons.
●Three of the four had coronary artery disease on autopsy, although none had a previous infarction.
Thus, the incidence of SCD in marathon runners is very low, and in this population, it appears unlikely that even a carefully taken medical history or routine screening with an electrocardiogram (ECG) or echocardiogram would have revealed potential risk.
Although the incidence of SCD among marathon runners is low (one death per 215,000 hours), it is higher than for other types of exercise, such as noncompetitive jogging (one death per 396,000 hours), cross-country skiing (one death per 607,000 hours), or general, noncompetitive exercise (one death per 375,000 hours) [10-13].
Coronary heart disease — In patients over age 35, the most frequent cause of exercise-related SCD is CHD. Ventricular arrhythmias can originate from myocardial scar (from prior myocardial infarctions), or from acute ischemia. In addition, ischemia during exertion can result either from fixed, chronic coronary stenoses that preclude increased myocardial oxygen delivery during exercise (ie, demand ischemia), or from an acute coronary syndrome. Autopsy examination of adults with exercise-related SCD usually reveals advanced CHD and/or an acute coronary lesion [20,57]. (See "Pathophysiology and etiology of sudden cardiac arrest" and "The role of the vulnerable plaque in acute coronary syndromes".)
Risk assessment — There are no data that directly relate the presence and severity of CHD to the risk of participating in competitive athletics. However, it is likely that the risk of a cardiac event during exercise increases with the presence of increasingly severe CAD, LV dysfunction and ventricular arrhythmias, as well as with the intensity of the competitive sport and the individual's effort. As a result, risk assessment should involve a full evaluation of cardiac status.
Prior to initiating systematic training or competition, athletes with previously documented CAD should have an assessment of LV function using echocardiography or radionuclide scanning. Exercise testing with perfusion imaging or echocardiography should be done, both to assess exercise capacity and to determine the extent of ischemia. Whenever possible, such testing should be performed while the patient is taking prescribed medications and should approximate the cardiovascular and metabolic demands of the planned athletic activity. (See "Cardiac rehabilitation: Indications, efficacy, and safety in patients with coronary heart disease".)
On the basis of the above testing, subjects can be risk stratified into those with a minimally increased or markedly increased risk.
Athletes with CHD are at minimally increased risk if all of the following are true:
●LV ejection fraction (LVEF) ≥50 percent.
●Normal exercise tolerance for age.
●No inducible ischemia with exercise testing.
●No sustained or nonsustained VT during exercise testing.
●No hemodynamically significant coronary artery stenoses if angiography is performed. Patients who have had successful revascularization of prior stenoses are also considered to be at low risk.
Athletes with CHD are at substantially increased risk if any of the above features are abnormal.
Competitive athletes — The following recommendations are based upon the 2005 36th Bethesda Conference on athletes and cardiovascular abnormalities [38]:
●Athletes with a minimally increased risk can participate in low dynamic and low/moderate static competitive sports (classes IA and IIA) (figure 1) but should avoid intensely competitive sports.
●Selected athletes with mildly increased risk may be permitted to compete in sports of higher levels of intensity when their overall clinical profile suggests very low exercise risk. This is particularly true for athletes in whom the only indication that coronary atherosclerosis is present is from an EBCT performed for screening purposes, and in which the total coronary calcium score is relatively low (ie, <15). All athletes should understand that the risk of a cardiac event with exertion is probably increased once coronary atherosclerosis of any severity is present.
●Athletes with mildly increased risk engaging in competitive sports should undergo re-evaluation of their risk stratification at least annually.
●Athletes in the substantially increased risk category should generally be restricted to low-intensity competitive sports (class IA) (figure 1).
●Athletes should be informed of the nature of prodromal symptoms (such as chest, arm, jaw and shoulder discomfort, unusual dyspnea) and should be instructed to cease their sports activity promptly and to contact their clinician if symptoms appear. Clinicians should be aware that competitive athletes may minimize symptoms that occur during exertion.
●Those with a recent MI or myocardial revascularization should cease their athletic training and competition until recovery is deemed complete. This interval varies among patient groups and depends upon the severity of the cardiovascular event and the success of revascularization. Such patients may benefit from cardiac rehabilitation during the recovery period. No firm guidelines exist for how long patients should avoid vigorous exercise training, but in general, patients post-stent placement for stable CAD symptoms should avoid vigorous exercise training for competition for approximately four weeks. Patients undergoing stent placement for unstable disease should wait at least this long. Following coronary bypass surgery, patients should avoid vigorous training until their incisions can tolerate vigorous activity.
●All athletes with atherosclerotic CAD should have their atherosclerotic risk factors aggressively treated as studies suggest that comprehensive risk reduction is likely to stabilize coronary lesions and may reduce the risk of exercise-related events.
Recreational athletes — Guidelines for recreational sports and exercise for patients with CHD are discussed in detail separately. (See "Exercise and fitness in the prevention of cardiovascular disease" and "Cardiac rehabilitation programs".)
SUMMARY AND RECOMMENDATIONS
●Sudden cardiac death (SCD) associated with athletic activity is a rare but devastating event. The majority of SCD events in athletes are due to malignant arrhythmias, usually ventricular tachycardia (VT) degenerating into ventricular fibrillation (VF), or primary VF itself. (See 'Introduction' above.)
●The balance between the risks and benefits of athletic activity depends upon several factors, including the presence and nature of cardiac disease, baseline fitness level in the individual, and the nature and intensity of athletic activity. Although there are some exceptions, for most individuals, the overall benefits of regular exercise far outweigh the risks. (See 'Balance of risks and benefits' above.)
●The literature on SCD during exertion has largely focused on competitive athletics. However, recreational activity limitations are also important in individuals with one of the cardiovascular diseases commonly associated with SCD. (See 'Recreational athletes' above.)
●The incidence of SCD among competitive athletes is actually quite low, estimated to be between 1 per 50,000 athletes to 1 per 300,000 athletes. (See 'Incidence of sudden death' above.)
●The potential etiologies of SCD include structural heart disease, inherited arrhythmias syndromes, and coronary heart disease; the exact distribution of etiologies varies according to age and geography, among other variables. (See 'Etiology of sudden death' above and "Pathophysiology and etiology of sudden cardiac arrest".)
●Some level of activity restriction (figure 1) is recommended for nearly all individuals with underlying heart disease. The precise restrictions vary depending on the underlying disease process and other comorbidities. (See 'Structural abnormalities associated with SCD' above and 'Inherited arrhythmia syndromes' above and 'Coronary heart disease' above.)
Use of UpToDate is subject to the Subscription and License Agreement.
REFERENCES
1.Thompson PD, Franklin BA, Balady GJ, et al. Exercise and acute cardiovascular events placing the risks into perspective: a scientific statement from the American Heart Association Council on Nutrition, Physical Activity, and Metabolism and the Council on Clinical Cardiology. Circulation 2007; 115:2358.
2.Maron BJ, Chaitman BR, Ackerman MJ, et al. Recommendations for physical activity and recreational sports participation for young patients with genetic cardiovascular diseases. Circulation 2004; 109:2807.
(I cut out the other references but can list them if anyone wants)
I offer this other recent article for further information to chew on.
http://www.acc.org/...y-disease-in-masters Prevalence of Subclinical Coronary Artery Disease in Masters Endurance Athletes With a Low Atherosclerotic Risk Profile
Ahmed Merghani, Viviana Maestrini, Stefania Rosmini, Andrew T. Cox, Harshil Dhutia, Rachel Bastiaenan, Sarojini David, Tee Joo Yeo, Rajay Narain, Aneil Malhotra, Michael Papadakis, Mathew G. Wilson, Maite Tome, Khaled AlFakih, James C. Moon, Sanjay Sharma
Download PDF Abstract
Background: Studies in middle-age and older (masters) athletes with atherosclerotic risk factors for coronary artery disease report higher coronary artery calcium (CAC) scores compared with sedentary individuals. Few studies have assessed the prevalence of coronary artery disease in masters athletes with a low atherosclerotic risk profile.
Methods: We assessed 152 masters athletes 54.4±8.5 years of age (70% male) and 92 controls of similar age, sex, and low Framingham 10-year coronary artery disease risk scores with an echocardiogram, exercise stress test, computerized tomographic coronary angiogram, and cardiovascular magnetic resonance imaging with late gadolinium enhancement and a 24-hour Holter. Athletes had participated in endurance exercise for an average of 31±12.6 years. The majority (77%) were runners, with a median of 13 marathon runs per athlete.
Results: Most athletes (60%) and controls (63%) had a normal CAC score. Male athletes had a higher prevalence of atherosclerotic plaques of any luminal irregularity (44.3% versus 22.2%;
P=0.009) compared with sedentary males, and only male athletes showed a CAC ≥300 Agatston units (11.3%) and a luminal stenosis ≥50% (7.5%). Male athletes demonstrated predominantly calcific plaques (72.7%), whereas sedentary males showed predominantly mixed morphology plaques (61.5%). The number of years of training was the only independent variable associated with increased risk of CAC >70th percentile for age or luminal stenosis ≥50% in male athletes (odds ratio, 1.08; 95% confidence interval, 1.01–1.15;
P=0.016); 15 (14%) male athletes but none of the controls revealed late gadolinium enhancement on cardiovascular magnetic resonance imaging. Of these athletes, 7 had a pattern consistent with previous myocardial infarction, including 3(42%) with a luminal stenosis ≥50% in the corresponding artery.
Conclusions: Most lifelong masters endurance athletes with a low atherosclerotic risk profile have normal CAC scores. Male athletes are more likely to have a CAC score >300 Agatston units or coronary plaques compared with sedentary males with a similar risk profile. The significance of these observations is uncertain, but the predominantly calcific morphology of the plaques in athletes indicates potentially different pathophysiological mechanisms for plaque formation in athletic versus sedentary men. Coronary plaques are more abundant in athletes, whereas their stable nature could mitigate the risk of plaque rupture and acute myocardial infarction.
Dale